THE ANATOMY OF STRESS
WHAT IS STRESS?
Stress can be defined as the body’s response to any external stimulus that causes a detectable and measurable, physical, psychological and or emotional response leading to altered function.
SIGNS AND SYMPTOMS OF STRESS?
- Neck, shoulders, and back pain.
- Neck, shoulders and back stiffness.
- Headaches. Most commonly, the headache will start at the base of the skull and then move upwards and forwards, covering the temples and ending in and above the eyes.
- Dizziness and vertigo.
- Balance problems.
- Abnormal bowel movements. Eg, Constipation.
- Insomnia. Difficulty falling asleep as well as interrupted sleep.
- Excessive sweating.
- Visual disturbances.
- High blood pressure and increased pulse rate.
- Irritability and explosive anger outbursts.
- Chronic fatigue and listlessness.
- Muscle cramps.
- Lack of concentration.
These are but a few of the reported and noted reactions to chronic exposure to stressful stimuli. If you recognise any of these, you may be suffering from stress-related dis-ease (a state of "not at ease," meaning the nervous system is not functioning properly, even if no symptoms are yet felt. It is considered the root cause of dysfunction.
Before I can discuss the anatomy of stress, I would like to describe all the individual components involved in the response pathway.
Auditory and visual stimuli:
Sights and sounds are processed first by the thalamus and then routed to the amygdala or the appropriate part of the cortex.
Olfactory and tactile stimuli:
Smell and touch sensations bypass the thalamus in totality and take a shortcut directly to the amygdala. Smells will therefore evoke stronger memories or feelings than do sights or sounds.
Thalamus:
The thalamus is the body's sensory integrative centre. Compare the thalamus to a railway shunting station. The thalamus breaks down incoming visual cues into shapes, colour, and size, and auditory cues into volume and dissonance, then routes the altered info to the cortex.
Cortex:
Gives meaning to all incoming information, enabling the brain to become conscious of what it sees and hears. One part of the prefrontal cortex is responsible for deactivating the stress-anxiety response once the initial threat has passed.
Amygdala:
The brain's emotional core is primarily responsible for triggering the stress response. Information that passes through the amygdala is tagged with emotional significance.
The Bed Nucleus of the Stria-Terminalis(BNST) :
The BNST takes information from the amygdala and magnifies it exponentially. It therefore perpetuates the cycle and prolongs the stress-anxiety state.
Locus Coeruleus:
Receives the emergency signal via the amygdala/BNST pathway and initiates the emergency response.
Once activated, the hypothalamus and pituitary glands will stimulate the adrenal glands to release large amounts of cortisol and adrenaline into the bloodstream. The stress hormones are broken down and absorbed extremely quickly, resulting in an almost instantaneous response from the target organs.
As a result of this pathway, the “fight, fright or flight “ (FFF) status is reached.
HOW DOES IT WORK?
When we are exposed to a severely stressful stimulus over time, depending on its magnitude, the body will initiate two defence pathways aimed at survival.
SHORTCUT :
The brain automatically engages an emergency hotline to its fear centre, the amygdala. The amygdala sends an all-points bulletin to all the structures in the emergency protocol pathway. The BNST further amplifies the emergency signal and sends it to the Locus Coeruleus. The LC activates the FFF via the stress hormones released by the adrenal glands.
Once the fight, fright, or flight response has been triggered, the body experiences a condition known as sympathetic excess. In other words, the sympathetic nervous system has taken over control. The body will show the following changes.
Increased heart rate and breathing.
Senses become hyper alert.
Increased blood supply to skeletal muscle prepares the muscle to react.
Digestion shutdown. The body could initially empty the digestive tract through vomiting, urination and defecation, or the peristaltic movement can totally decrease, leading to constipation.
Blood pressure will rise, and lungs will hyperinflate.
Increased sweating.
Peripheral nerves will tingle into action, creating goose bumps.
THE HIGH ROAD:
Only after the fear response has been triggered does the conscious mind kick into gear. Some sensory information will take the longer route and first go to the thalamus. The thalamus will organise the information and route it to the appropriate part of the cortex. The cortex will now analyse all the raw data and decide whether the fear response was necessary. If the cortex feels that the response is validated, it will order the fear centre (amygdala) to continue with the emergency response. If not, the cortex will order the amygdala to stand down and to deactivate.
WHAT HAPPENS IF THE CORTEX IS NOT ABLE TO DE-ACTIVATE THE AMYGDALA?
Prolonged FFF leads to anxiety.
Prolonged anxiety leads to sympathetic excess.
Prolonged stress can contribute to fatigue, poor sleep, muscle tension, pain sensitivity, reduced resilience, and tissue damage.
Tissue damage leads to altered function, dis-ease and disability.
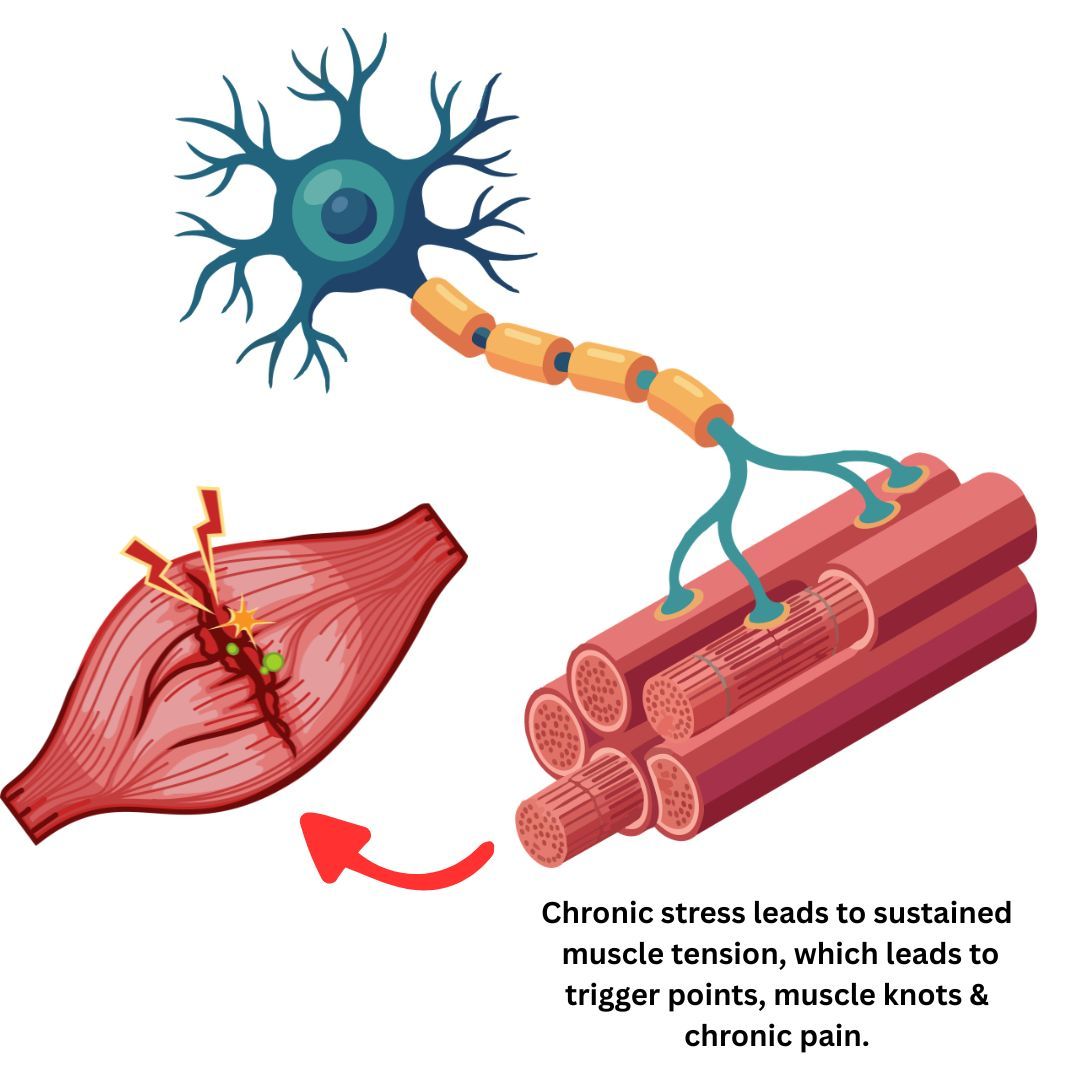
Sustained muscle contraction starves the muscle fibres of oxygen and damages the delicate structures inside them.
Over time, this produces the trigger points, muscle knots and chronic pain that we as chiropractors see in our patients every day.
The cycle is reversible. Once you remove the stress driver and the nervous system rebalances, the muscles recover and function returns. The question is how to break the cycle in the first place.
Stressor
A mental, physical, emotional or postural trigger.
Stress response activated
Your brain triggers fight, fright or flight (FFF).
Stress hormones surge
Cortisol and adrenaline flood the bloodstream.
when the stress does not switch off…
Muscles tighten and stay tight
Sustained contraction with no chance to recover.
Tissue micro-damage
Trigger points, knots and inflammation develop.
Pain, dysfunction, dis-ease
Reduced mobility, chronic symptoms, lower quality of life.
The good news: the cascade is reversible. Once you remove the stress driver and the nervous system rebalances, your muscles recover and function returns.
HOW CAN WE DE-STRESS?
The theory in this case is much easier said than done. Because we all act and react differently to stress, the mechanism to de-stress remains personal. The first step must always be a baby step with the primary aim of breaking the stress-anxiety cycle. Remember the opening statement: we are never too old to learn, and we are never too old to change.
I have summarised 10 easy baby steps for you to adopt into your daily routine. If you change your attitude and consciousness towards stress and truly understand the underlying mechanism, you have already taken the first step. Good luck with the rest!
1. Identify the stimulus or stimuli in your personal life responsible for your stress. Once you have made that identification, confront that stimulus head-on. Don’t run, don’t hide, because the mechanism is already there, and you can’t run or hide from it. Only when your conscious mind perceives the stimulus as no longer threatening will the amygdala be deactivated. The two most common stress-inducing stimuli in the workplace today are unfinished tasks and unresolved conflict.
2. Start your day with a positive thought. So often will the mood or the platform for the new day be dictated by the first thought that we have when we wake up. Make it a positive one, even if you have to cheat a little. Write something down the previous evening and put it next to your bed.
3. Verbalise your positive thought. Share it with your wife, girlfriend, boyfriend or talk to yourself in the mirror.
4. Apply that positive emotion. Smile at someone in traffic, be friendly at the office, and phone someone and say something nice.
5. Eat three fruits every day. Baby steps.
6. Exercise three times per week. Baby steps. Start slowly.
7. Stretch three times per day. Make time for yourself. Force yourself to relax for five minutes every hour. Sit back and stretch!
8. Stimulate yourself intellectually outside the work environment. Read, learn or start an interesting hobby. Don’t stagnate!
9. Learn to relax. Start doing yoga, listen to music or go for a massage. Spoil yourself.
10. Learn to be proactive when it comes to your health. Don’t wait until you have neck or back pain to visit your chiropractor. Don’t wait until you have a muscle spasm before you visit your physiotherapist. Don’t wait for the symptoms of a cold and flu to force you to go to your GP. Don’t work without a break until your body breaks down and forces you to rest. The health paradox of our time is negative reinforcement. We only rest or react once we are already sick or sore; therefore, we reward our bodies for being sick. Reward your body for the positive things that it does for you. Reward yourself constantly!
This article is for general education only. Persistent dizziness, unexplained high blood pressure, severe headaches, chest pain, fainting, or ongoing fatigue should be assessed by a medical doctor.